Prevention and management of healthcare-associated issues related to vascular devices is high priority
Phlebitis matters “I hate hospitalization. I particularly get anxious about the insertion of needles for IV fluids because it makes the area blue and painful for many days.” These are words one often hears from people
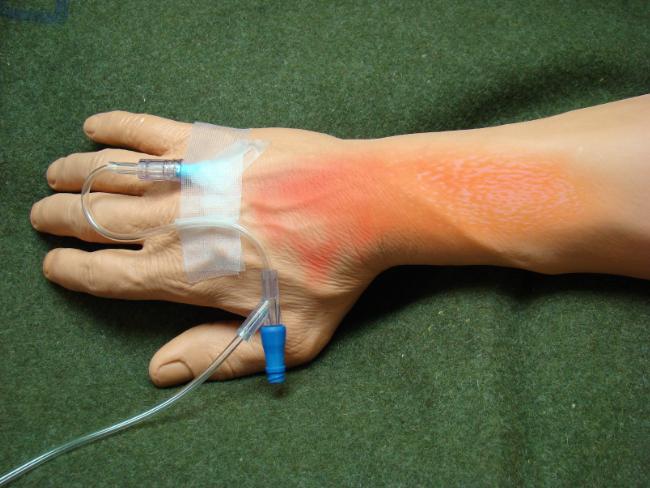
Phlebitis matters
“I hate hospitalization. I particularly get anxious about the insertion of needles for IV fluids because it makes the area blue and painful for many days.” These are words one often hears from people who have been hospitalized. It is not surprising as it has been reported that more than 1 in 2 people worldwide who have undergone peripheral intravenous catheterization (PIVC) experience phlebitis.1In India too, this incidence is almost 1 in 3 (31%).2
While peripheral intravenous catheterization (PIVC) is the most common and the first life-saving procedure performed on nearly 70% of hospitalized patients around the world, its frequent use can lead to complications such as blockages, dislodgements, redness, swelling, infections, etc., in nearly 50% of the cases. Such complication scan cause not only pain but also extreme distress to patients.
A National Study of Adverse Events (ENEAS, acronym in Spanish) 3 reports that if phlebitis were included as an adverse healthcare event, it would rank first followed by medication errors, infections arising from healthcare practices and surgical techniques. No wonder patients often tend to avoid certain hospitals where they have had a bad experience of phlebitis, harming the reputation of the doctor and the hospital.
PIVC insertion practices and Impact on Healthcare
The prevention and management of healthcare-associated issues related to invasive devices have become a high priority patient safety protocol in recent times. It is important to ensure that good clinical practices are in place to improve every aspect of the patient’s overall hospital experience. This will also uphold the reputation of the doctors, nurses and hospitals.
The use of irritating solutions, not allowing skin antisepsisto dry, inadequate haemodilution, improper catheter size orstabilization technique, breaks in aseptic technique and non-occlusive dressing could cause phlebitis.4
Vascular access management for reduction of phlebitis
It is important to know the risks and integrate good practices in vascular access device management.
- Ensure thorough cleaning of the clinician’s and nurse’s hands; wearing gloves and cleaning the patient’s skin adequately should be followed
- Attention should be given to the IV sites of patients who are under recurrent IV therapy as consistent use of the site may increase the risk of bacterial phlebitis
- An appropriate vascular device should be selected for the vein, and use the right devices that are protected.
- The site at which the device is inserted should be properly selected to avoid any bony portions, joints and valves that may lead to the device moving within the vein and causing phlebitis
- Proper attention and dressing should be done after insertion of the vascular device into the vein. This willreduce the incidence of phlebitis as opposed to using tape to secure the device.
Prevention is the best remedy for all vascular access management complications. The easiest way
to achieve this is to invest in innovative vascular access devices and adopt globally recommended
best practices. After all, you will always want to be in touch with the best devices and practices
when it is a matter of life, patient satisfaction and hospital reputation.
————————————————————————————
References
1.Takahashi, T., Murayama, R.,et al., 2020.Preventing peripheral intravenous catheter failure by reducing mechanical irritation. Scientific Reports, 10(1).
2.Raghu, K. and Mandal, A., 2019. Study on incidence of phlebitis following the use of pherpheral intravenous catheter. Journal of Family Medicine and Primary Care, 8(9), p.2827.
- Guanche-Sicilia, A., Sánchez-Gómez, M.,et al., 2021. Prevention and Treatment of Phlebitis Secondary to the Insertion of a Peripheral Venous Catheter: A Scoping Review from a Nursing Perspective.Healthcare, 9(5), p.611.
- Infusion Therapy Standards of Practice. J InfusNurs. 2021; 8th Edition : S 211






